Mumps: Causes, Symptoms, Complications and Treatment
- 1. Mumps Kuldeep Vyas Asst. Prof. Community Health Nursing
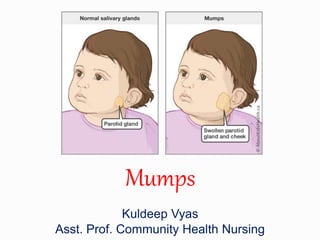
- 2. Definition Kuldeep Vyas M.Sc. CHN 25-06-2020 2 Mumps is an acute viral infection of childhood that typically involves swelling of one or both parotid glands, although many different organs can be infected.
- 3. Etiology Kuldeep Vyas M.Sc. CHN 25-06-2020 3 Mumps virus, the cause of mumps, is an RNA virus of the genus Rubulavirus in the Paramyxoviridae family , which also includes the parainfluenza viruses. Only one serotype is known
- 4. Epidemiology Kuldeep Vyas M.Sc. CHN 25-06-2020 4 Mumps is endemic in most unvaccinated populations The virus is spread from human reservoir by ; * Direct contact * Airborne droplets * Fomites contaminated by saliva * possibly by urine It is distributed worldwide Affects both sexes equally
- 5. Epidemiology (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 5 Before introduction of the vaccine in 1967: * the peak incidence of the disease occurred in children 5-9 yr of age * 85% of infections occurred in children younger than 15 yr of age. Now most cases occur in young adults, producing outbreaks in colleges or in the workplace.
- 6. Epidemiology (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 6 Outbreaks appear to be primarily related to a lack of immunization, especially in an underimmunized cohort of children born from 1967-1977, rather than to waning to immunity. Epidemics occur at all seasons but are slightly more frequent in late winter and spring.
- 7. Epidemiology (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 7 In the United States, the reported incidence of mumps declined after the introduction of mumps vaccine in 1967 the recommendation for its routine use in 1977. After expanded recommendations for a 2- dose measles, mumps, and rubella (MMR) vaccine schedule for measles control in 1989, mumps cases declined further
- 8. Reported cases of mumps infection per 100 000 population, 1978–2003. (Data from Centers for Disease Control and Prevention. Summary of notifiable diseases, United States 2003. MMWR 2005;52: 54.) Kuldeep Vyas M.Sc. CHN 25-06-2020 8
- 9. Epidemiology (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 9 Virus has been isolated from saliva as long as 6 days before and up to 9 days after appearance of salivary gland swelling. Transmission does not seem to occur more than 24 hr before the appearance of the swelling or later than 3 days after it has subsided. Virus has been isolated from urine from the 1st- 14th day after the onset of salivary gland swelling.
- 10. Pathogenesis Kuldeep Vyas M.Sc. CHN 25-06-2020 10 After entry into the last and initial multiplication in the cells of the respiratory tract, the virus is bloodborne to many tissues, among which the salivary and other glands are the most susceptible.
- 11. Clinical Manifestations Kuldeep Vyas M.Sc. CHN 25-06-2020 11 The incubation period ranges from 14-24 days, with a peak at 17-18 days. Approximately 30-40% of infections are subclinical In children, prodromal manifestations are rare but may be manifest by: * Fever * Muscular pain (especially in the neck) * Headache * Malaise typically precede the parotid swelling by 12 to 24 hours
- 12. Clinical Manifestations (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 12 *Common complaints are: Earache on the side of parotid involvement Discomfort with eating or drinking acidic food * Parotid pain is most pronounced during the first few days of swelling
- 13. Clinical Manifestations (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 13 The swollen parotid gland lifts the earlobe upward and outward, and the angle of the mandible is obscured the opening of the Stensen duct on the buccal mucosa is edematous and erythematous. Trismus (spasm of the masticatory muscles) can occur.
- 14. Toddler with mumps parotitis (Courtesy of A. Margileth.) Kuldeep Vyas M.Sc. CHN 25-06-2020 14
- 15. Clinical Manifestations (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 15 Other salivary glands such as the submandibular and sublingual glands may also be involved. In 10-15% of patients only the submandibular gland(s) may be swollen Presternal edema can be notable. Morbilliform rash has been reported in association with mumps infection
- 16. Clinical Manifestations (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 16 Systemic symptoms, including fever, usually resolve within 3 to 5 days the parotid swelling subsides within 7 to 10 days Adolescents and adults have more severe disease than young children.
- 17. Diagnosis Kuldeep Vyas M.Sc. CHN 25-06-2020 17 The diagnosis of mumps parotitis is usually apparent from the clinical symptoms and physical examination Routine laboratory tests are nonspecific; usually leukopenia is present with relative lymphocytosis. An elevation in serum amylase levels is common; the rise tends to parallel the parotid swelling and then to return to normal within 2 wk
- 18. Diagnosis (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 18 The microbiologic diagnosis is by serology or virus culture Enzyme immunoassay for mumps immunoglobulin (Ig). IgG and IgM antibodies are most commonly used for diagnosis. IgM antibodies are detectable in the first few days of illness and are considered diagnostic
- 19. Diagnosis (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 19 Mumps virus can be cultured from the saliva, cerebrospinal fluid, blood, urine, brain, and other infected tissues. Primary cultures of human or monkey kidney cells are used for viral isolation The mumps skin test is unreliable for diagnosis of mumps and for determination of susceptibility to infection.
- 20. DIFFERENTIAL DIAGNOSIS Kuldeep Vyas M.Sc. CHN 25-06-2020 20 The differential diagnosis of parotitis is broad and includes: bacterial (suppurative) parotitis parotid duct stone drug reactions recurrent parotitis of childhood Other viruses, such as influenza, coxsackievirus A, echovirus, and parainfluenza viruses 1 and 3, can cause parotitis and are usually responsible for “recurrent mumps” parotid tumor Sjögren syndrome
- 21. Kuldeep Vyas M.Sc. CHN 25-06-2020 21 viru s. (Courtesy of J.H. Brien.)
- 22. Treatment Kuldeep Vyas M.Sc. CHN 25-06-2020 22 There is no specific antiviral therapy; treatment is entirely supportive. Antipyretics (acetaminophen or ibuprofen) are indicated for fever. Bed rest should be guided by the patient's needs, but no evidence indicates that it prevents complications. The diet should be adjusted to the patient's ability to chew.
- 23. Treatment(cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 23 Orchitis should be treated with local support and bed rest. Mumps arthritis may respond to a 2-wk course of a nonsteroidal anti-inflammatory agent or corticosteroids. Salicylates do not appear to be effective
- 24. Complications Kuldeep Vyas M.Sc. CHN 25-06-2020 24 MENINGOENCEPHALOMYELITIS 1.The most frequent complication in childhood 2.Clinical manifestations occur in more than 10% of patients 3.The incidence of mumps meningoencephalitis is approximately 250/ 100,000 cases 4. The mortality rate is about 2%
- 25. Complications Kuldeep Vyas M.Sc. CHN 25-06-2020 25 MENINGOENCEPHALOMYELITIS (cont.) 5. may be either: I. Primary infection of neurons: parotitis frequently appears at the same time or following the onset of encephalitis II. Postinfectious encephalitis with demyelination : encephalitis follows parotitis by an average of10 days.
- 26. Complications Kuldeep Vyas M.Sc. CHN 25-06-2020 26 MENINGOENCEPHALOMYELITIS (cont.) *Mumps meningoencephalitis is clinically indistinguishable from meningoencephalitis of other origins * Moderate stiffness of the neck is seen, but the remaining findings on neurologic examination are usually normal *The cerebrospinal fluid may show a lymphocytic pleocytosis of less than 500 cells/ mm3, although occasionally the count may exceed 2,000 cells/mm3.
- 27. Complications (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 27 ORCHITIS AND EPIDIDYMITIS 1. These complications rarely occur in prepubescent boys but are common (14-35%) in adolescents and adults. 2. The testis is most often infected with or without epididymitis; epididymitis may also occur alone. 3. Bilateral orchitis occurs in approximately 30% of patients. Rarely, there is a hydrocele. 4.The orchitis usually follows parotitis within 8 days. Orchitis may also occur without evidence of salivary gland infection. .
- 28. Complications Kuldeep Vyas M.Sc. CHN 25-06-2020 28 ORCHITIS AND EPIDIDYMITIS (cont.) 5.The onset is usually abrupt, with a rise in temperature, chills, headache, nausea, and lower abdominal pain; 6. The affected testis becomes tender and swollen, and the adjacent skin is edematous and red. 7.The average duration of illness is 4 days. 8. Approximately 30-40% of affected testes atrophy, leaving a cosmetic imbalance. 9. Infertility is rare even with bilateral orchitis.
- 29. Complications (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 29 OOPHORITIS Pelvic pain and tenderness are noted in about 7% of postpubertal female patients. There is no evidence of impairment of fertility.
- 30. Complications (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 30 PANCREATITIS * Mild or subclinical pancreatic involvement is common, but severe pancreatitis is rare. * It may be unassociated with salivary gland manifestations and may be misdiagnosed as gastroenteritis. * Epigastric pain and tenderness, which are suggestive, may be accompanied by fever, chills, vomiting, and prostration. * An elevated serum amylase value is characteristically present in patients with mumps, with or without clinical manifestations of pancreatitis
- 31. Complications (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 31 MYOCARDITIS *Serious cardiac manifestations are extremely rare * mild infection of the myocardium may be more common than is recognized. * Electrocardiographic tracings revealed changes, mostly depression of the ST segment, in 13% of adults in one series. * Such involvement may explain the precordial pain, bradycardia, and fatigue sometimes noted among adolescents and adults with mumps.
- 32. Complications (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 32 ARTHRITIS *Migratory polyarthralgia and even arthritis are occasionally seen in adults with mumps but are rare in children. *The knees, ankles, shoulders, and wrists are most commonly affected. *The symptoms last from a few days to 3 mo, with a median duration of 2 wk
- 33. Complications (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 33 THYROIDITIS * It is uncommon in children * A diffuse, tender swelling of the thyroid may occur about 1 wk after the onset of parotitis * Antithyroid antibodies subsequently develop
- 34. Complications (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 34 DEAFNESS * Unilateral, rarely bilateral, nerve deafness may occur * the incidence is low (1/15,000 cases) * mumps was historically a leading cause of unilateral nerve deafness. * The hearing loss may be transient or permanent.
- 35. Complications (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 35 OCULAR COMPLICATIONS * Dacryoadenitis may occur with painful swelling, usually bilateral, of the lacrimal glands. * Optic neuritis (papillitis) may occur *Symptoms vary from loss of vision to mild blurring, with recovery in 10-20 days.
- 36. Prognosis Kuldeep Vyas M.Sc. CHN 25-06-2020 36 The prognosis of mumps in childhood is excellent. Infection usually confers permanent immunity Reinfections have been documented
- 37. Prevention Kuldeep Vyas M.Sc. CHN 25-06-2020 37 Mumps vaccine is derived from the Jeryl Lynn strain of mumps virus, The vaccine induces antibody in 96% of seronegative recipients and has 97% protective efficacy. The initial mumps immunization, usually as measles- mumps-rubella (MMR) vaccine, is recommended at 12- 15 mo of age. A second immunization, also as MMR, is recommended routinely at 4-6 yr of age but may be administered at any time during childhood provided at least 4 wk have elapsed since the first dose.
- 38. Prevention (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 38 Women should avoid becoming pregnant for 30 days after monovalent mumps vaccination (3 mo if vaccination was performed with rubella vaccine). Other contraindications to vaccination include: *allergy to a vaccine component (anaphylaxis to neomycin) * moderate or severe acute illnesses with or without fever *immunodeficiency (primary immunodeficiencies, cancer and cancer therapy, long-term high-dose corticosteroid therapy, severely immunocompromised, including those with HIV infection)
- 39. Prevention (cont.) Kuldeep Vyas M.Sc. CHN 25-06-2020 39 Children who have not previously received the second dose should be immunized by 11-12 yr of age. Rarely, parotitis and low-grade fever can develop 10-14 days after vaccination. Vaccinees do not shed virus. Maternal antibody is protective in the infant in the first 6 mo of life.
- 40. Summary Kuldeep Vyas M.Sc. CHN 25-06-2020 40 Mumps is an acute viral infection involves swelling of one or both parotid glands Mumps is an RNA virus of the genus Rubulavirus in the Paramyxoviridae family spread from human reservoir by ; direct contact. airborne droplets. fomites contaminated by saliva and possibly by urine Transmission does not seem to occur more than 24 hr before the appearance of the swelling or later than 3 days after it has subsided The incubation period ranges from 14-24 days, with a peak at 17-18 days. Approximately 30-40% of infections are subclinical Common complaints are: earache ,discomfort with eating or drinking acidic food parotid pain is most
- 41. Summary Kuldeep Vyas M.Sc. CHN 25-06-2020 41 the opening of the Stensen duct on the buccal mucosa is edematous and erythematous. submandibular and sublingual glands may also be involved. the parotid swelling subsides within 7 to 10 days The diagnosis of mumps parotitis is usually apparent from the clinical symptoms and physical examination There is no specific antiviral therapy; treatment is entirely supportive. Complications include: MENINGOENCEPHALOMYELITIS, ORCHITIS AND EPIDIDYMITIS, OOPHORITIS , PANCREATITIS , MYOCARDITIS, ARTHRITIS , THYROIDITIS, DEAFNESS and OCULAR COMPLICATIONS The prognosis of mumps in childhood is excellent. Infection usually confers permanent immunity
- 42. Thank You…
